Peritonitis (Peritoneal Dialysis Related)
Disclaimer
These guidelines have been produced to guide clinical decision making for the medical, nursing and allied health staff of Perth Children's Hospital. They are not strict protocols, and they do not replace the judgement of a senior clinician. Clinical common-sense should be applied at all times. These clinical guidelines should never be relied on as a substitute for proper assessment with respect to the particular circumstances of each case and the needs of each patient. Clinicians should also consider the local skill level available and their local area policies before following any guideline.
Read the full CAHS clinical disclaimer
|
Aim
- To outline the roles and responsibilities of Emergency Department (ED) Staff and the Safety Team After-hours Response Service (STARS) in facilitating treatment of Peritoneal Dialysis (PD) patients with peritonitis symptoms.
- To outline the process for facilitating PD fluid sampling / intraperitoneal antibiotic administration, within 2 hours, in patients presenting to the ED with peritonitis symptoms.
Signs and symptoms
Peritonitis should be suspected in the child on PD who presents with the following:
Key points
- This procedure is to be utilised alongside the Peritoneal Dialysis: Management of Dialysis Related Infections (internal WA Health only), and the patient’s Individualised Peritonitis and Peritoneal Catheter Contamination Plan.
- All PD patients have an Individualised Peritonitis and Peritoneal Catheter Contamination Plan (MR 101.13) – this is located in the patient’s Digital Medical Record (DMR) in the Summary section.
- The plan has pre-calculated intraperitoneal antibiotic doses based on current / most recent weight for treatment of peritonitis and contamination of the PD catheter.
- Obtain copy of the plan from the DMR and discuss with Nephrologist on-call to determine the treatment plan.
- All PD patient parents or carers who manage their child’s PD at homeare educated to attend the ED for symptoms of peritonitis.
- The Nephrologist on-call is the first point of contact for suspected peritonitis management - contact through PCH switchboard on 08 6456 2222.
- Obtaining a fresh PD fluid drainage sample is the first step in treatment, followed by loading doses of intraperitoneal antibiotics delivered via PD as ordered by Nephrologist on-call.
- The PD fluid sample is to be obtained within 1 hour of presentation, followed by intraperitoneal antibiotics.
- All PD patients have a surgically implanted PD catheter for PD.
- Only PD competent trained staff are to access PD catheters and perform dialysis procedures.
- Competent staff include:
- Nurses who have undergone the required role-based training on Ward 4B
- STARS Clinical Nurse Specialists (CNS’s),
- Renal CNS’s, Renal Clinical Nurse
- Paediatric Critical Care Nurses.
Contacting the Renal Team
During business hours
- If patients or carers suspect peritonitis, they should contact the Renal CNS via PCH switchboard on 08 6456 2222. The renal CNS will advise them to attend ED and will notify ED of the expected patient.
- If a patient presents to ED unexpectedly, ED staff should contact the Nephrologist on-call via Switchboard and Renal CNS via Vocera or Extension 65376.
Outside of business hours
- If patients or carers suspect peritonitis, they should contact the on-call Nephrologist via the PCH switchboard on 08 6456 2222, who will advise they attend ED. The Nephrologist will advise ED and the STARS CNS of the expected patient.
- If a patient presents to ED unexpectedly, ED staff should contact the on-call Nephrologist via the PCH switchboard.
- ED Staff to refer to Peritonitis Presentation Outside Business Hours for management.
Assessment
- Refer to Management Pathway for Peritoneal Dialysis Peritonitis
- Treatment should commence within 2 hours of presentation.
- Complete and record a full set of observations on the age appropriate Observation and Response Tool and record additional information on the Clinical Comments chart.
- Escalate care according to the Early Warning Score Escalation pathway and the Paediatric Sepsis Pathway Trigger.
- Complete a general and abdominal examination. Note any swelling, tenderness or exudate from catheter tunnel or exit site.
- Assessment to exclude alternative causes of abdominal pain or fever.
- ED shift co-ordinator should contact Renal CNS / STARS CNS upon arrival of the patient to collect a PD sample.
- If medically stable, progress with PD fluid sampling, discuss need for blood test +/- IV access with Nephrologist.
- If medically unstable / sepsis / shock, treat as per Sepsis recognition and management. Do not delay antibiotics to obtain PD fluid sample.
Investigations
- Full Blood Picture (FBP), Urea, Electrolytes and Creatinine (UEC), C-Reactive Protein (CRP), blood cultures.
- Peritoneal dialysis fluid sample – Microscopy, Culture and Sensitivity (MC+S), Cell count and differential. Form should be marked “URGENT – please call on-call Nephrologist with cell count”. Call Microbiology lab to advise of urgent sample. See Management of Dialysis Related Infections (internal WA Health only) for instructions on taking PD fluid sample.
- Discuss findings with Nephrologist i.e. results; advise PD sample taken and clarity of drained fluid; patient condition; expected time to admission and administration of antibiotics.
Peritonitis presentation outside business hours
Outside business hours, the following staff need to be advised as soon as possible after the patient presents with suspected peritonitis.
1. Nephrologist on-call
- Discuss condition, confirm treatment required e.g. PD fluid sample, bloods, IV fluids.
- Advise Nephrologist when PD sample was taken, results of drainage microscopy, and if drainage cloudy or clear when sample taken.
- If peritonitis confirmed on microscopy – Update Nephrologist on bed status and of possible delays to transfer to Ward 4B, as IV antibiotics may need to be considered to cover until intraperitoneal antibiotics can be administered.
2. STARS CNS
- STARS CNS to be notified as soon as possible to attend ED to take PD sample for microscopy.
- Advise Ward 4B shift coordinator of presentation and request 2000 mL Stay safe® bag to be placed on warmer in preparation for the administration of intraperitoneal antibiotics on arrival to Ward 4B if not already administered.
- Refer to patient’s Individualised Peritonitis and Peritoneal Catheter Contamination Plan for the required glucose concentration Staysafe® bag (or discuss with Nephrologist).
- Take PD drainage sample using Manual Acute Set Up. Notify ED Consultant of clarity of fluid.
- If a drainage sample is unable to be obtained (e.g. child has dry abdomen), STARS CNS to use Manual Acute Set Up to deliver a fluid dwell. Call Nephrologist for instructions.
- Sample to be taken 2 hours after dwell.
- Administer intraperitoneal antibiotics in ED if patient unable to be transferred to the ward.
3. Hospital Clinical Manager (HCM)
- If STARS CNS unavailable for sample collection, discuss with HCM regarding the availability of PD competent staff to take sample.
- A stable patient can be expedited to Ward 4B for the sample to be taken and for the administration of intraperitoneal antibiotics if a bed is available.
- HCM to be advised as soon as the need for inpatient admission is confirmed to minimise any delay to treatment or transfer.
Ward 4B Shift Coordinator
- ED staff, STARS CNS or HCM to ensure the Ward 4B shift coordinator is informed of the patient’s presentation and that a 2000 mL Staysafe® bag has been placed on warmer for intraperitoneal antibiotics.
- Refer to patient’s Individualised Peritonitis and Peritoneal Catheter Contamination Plan for the required glucose concentration Staysafe® bag (or discuss with Nephrologist).
Management pathway for Peritoneal Dialysis Related Peritonitis
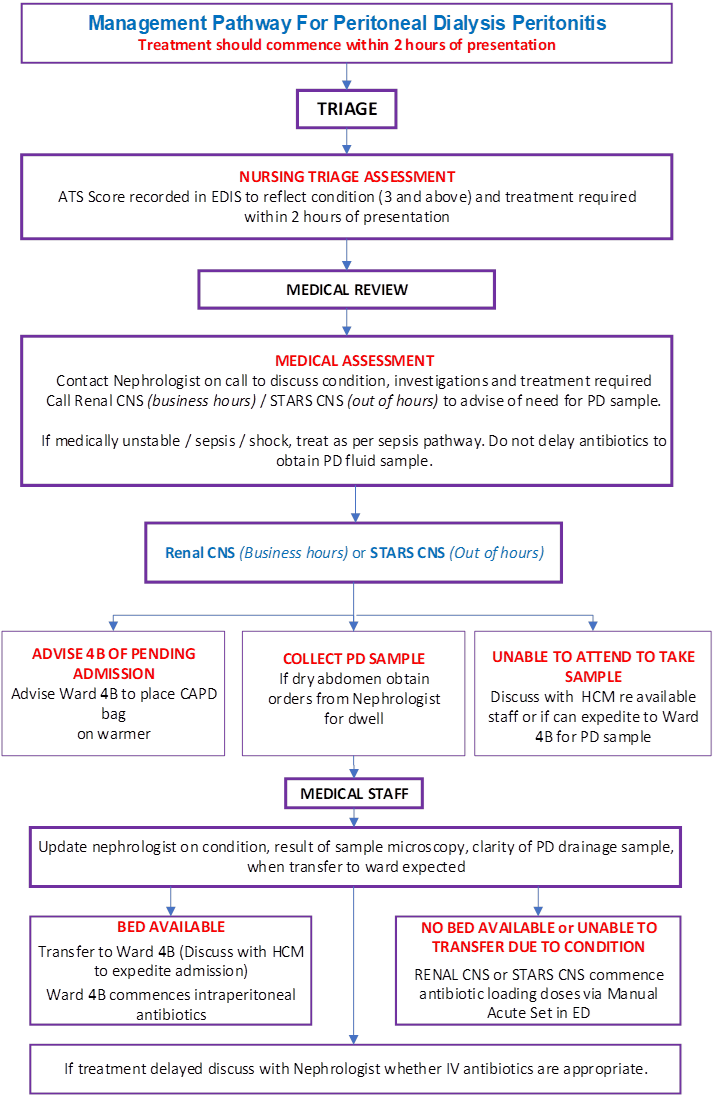
References
- Warady BA, Same R, Borzych-Duzalka D, Neu AM, El Mikati I, Mustafa RA, et al. Clinical practice guideline for the prevention and management of peritoneal dialysis associated infections in children: 2024 update. Perit Dial Int [Internet]. 2024 Sep 1;44 (5): 303-64. Available from https://pubmed.ncbi.nlm.nih.gov/39313225/
| Endorsed by: |
Co-director Surgical Services (Nursing) |
Date: |
Mar 2026 |
This document can be made available in alternative formats on request for people with disability.