Status epilepticus
Disclaimer
These guidelines have been produced to guide clinical decision making for the medical, nursing and allied health staff of Perth Children’s Hospital. They are not strict protocols, and they do not replace the judgement of a senior clinician. Clinical common-sense should be applied at all times. These clinical guidelines should never be relied on as a substitute for proper assessment with respect to the particular circumstances of each case and the needs of each patient. Clinicians should also consider the local skill level available and their local area policies before following any guideline.
Read the full CAHS Emergency Department disclaimer
|
Aim
To guide staff with the assessment and management of status epilepticus.
Definition
Convulsive status epilepticus is defined as a generalised tonic‐clonic convulsion lasting more than 30 minutes, or repeated tonic‐clonic convulsions over a 30 minute period without recovery of consciousness between each convulsion.
Background
- Status epilepticus is the most common neurological medical emergency
- In approximately 30% of cases, status epilepticus is the initial presentation of a seizure disorder
- Mortality is 1-3%.
Key points
The estimated incidence is 20 per 100,000 children per year.
Risk
Treatment delay is associated with increased morbidity and mortality.
Causes of Status epilepticus:
- prolonged febrile convulsion
- epilepsy
- central nervous system infection (e.g. meningitis)
- trauma
- metabolic
- poisons.
Assessment
History
- Description of the manifestation of the seizures obtained from the eyewitnesses (parent, carer, etc)
- Any impairment or loss of consciousness
- Motor effects, muscular contractions
- Parts of the body that are affected
- Focal or tonic/clonic seizure
- Length of seizure
- Multiple clusters of seizure activity.
Examination
- Full systems examination including neurological examination
- Examine for underlying causes that can precipitate seizures.
Investigations
- Always do a blood glucose level (BGL)
- Venous blood gas
- Consider other investigations according to the possible underlying aetiology e.g. infectious screen, anti-epileptic drug levels.
Management
- Assess ABC first
- The approach to a child who presents with a tonic-clonic convulsion > 5 minutes should be the same as for the child with established status epilepticus
- This guideline addresses the treatment of status epilepticus and not the underlying cause – once the seizure has been terminated, investigate as required
Initial management
- ABC
- Airway adjuncts – consider an oropharyngeal or nasopharyngeal airway as required
- High flow oxygen
- Vascular access (and check BGL)
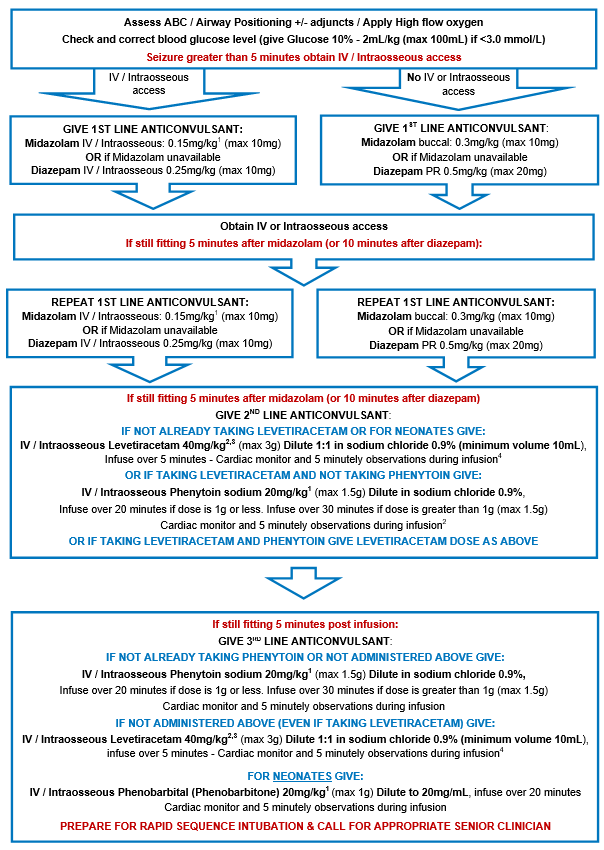
- Status epilepticus flowchart
Medications
See Seizure - Medication.
Nursing
- Follow the Status epilepticus flowchart and prepare drugs as required
- Any child having a prolonged seizure should be nursed in resuscitation room if possible
- Prepare to insert 2 x intravenous cannulae or intraosseous needles
- Check BGL and inform doctor.
Observations
Baseline observations
- Temperature
- Heart rate
- Respiratory rate
- Blood pressure
- GCS
- Pupil reaction.
During Levetiracetam, Phenobarbital (Phenobarbitone) or Phenytoin sodium Infusion
- 5 minutely blood pressure (BP), heart rate (HR), oxygen saturations (SpO2) respiratory rate (RR), for duration of infusion and for 30 minutes following completion of the flush.
- Advise doctor immediately if any change in patients condition
- Infusion may need to be slowed or stopped in case of hypotension, impaired respiratory effort or bradycardia.
Post Ictal stage
- Observe closely for further seizure activity
- 1/2 hourly neurological observations until GCS 15.
References
- AMH Children’s Dosing Companion. A-Z Medication Monographs. Australian Medicines Handbook Pty Ltd. Update Jan 2020. (Available via CAHS library)
- Dalziel S, Borland M, Furyk J, Bonisch M, Neutze J, et al. Levetiracetam versus phenytoin for second-line treatment of convulsive status epilepticus in children (ConSEPT): an open-label, multicentre, randomised controlled trial. The Lancet, 2019. doi.org/10.1016/S0140-6736(19)30722-6
- Lyttle M, Rainford N, Gamble C, Messahel S, Humphreys A, et al; with support of Paediatric Emergency Research in the United Kingdom & Ireland (PERUKI) collaborative* Levetiracetam versus phenytoin for second-line treatment of paediatric convulsive status epilepticus (EcLiPSE): a multicentre, open-label, randomised trial. The Lancet, 2019 http://dx.doi.org/10.101d6/S0140-6736(19)30724-X
- Wilfong A.. Management of convulsive status epilepticus in children. UpToDate: Wolters Kluwer; Updated Feb 2020. Accessed 01/04/2020
Bibliography
- Chin RF, Neville BG, Peckham Cet al. Incidence, cause, and short-term outcome of convulsive status epilepticus in childhood: prospective population-based study. Lancet 2006; 368: 222–9.
- Carey JM, Shah MI. Pediatric prehospital seizure management. Clin. Pediatr. Emerg. Med. 2014; 15:59–66.
- Raspall-Chaure M, Chin RF, Neville BG, Bedford H, Scott RC.The epidemiology of convulsive status epilepticus in children: a critical review. Epilepsia. 2007;48(9):1652.
- Raspall-Chaure M, Chin RF, Neville BGR, Scott RC. Outcome of paediatric convulsive status epilepticus: a systematic review. Lancet Neurol. 2006; 5: 769–79.
| Endorsed by: |
Drug and Therapuetics Commitee |
Date: |
Jul 2022 |
This document can be made available in alternative formats on request for a person with a disability.