Hand trauma
Disclaimer
These guidelines have been produced to guide clinical decision making for the medical, nursing and allied health staff of Perth Children’s Hospital. They are not strict protocols, and they do not replace the judgement of a senior clinician. Clinical common-sense should be applied at all times. These clinical guidelines should never be relied on as a substitute for proper assessment with respect to the particular circumstances of each case and the needs of each patient. Clinicians should also consider the local skill level available and their local area policies before following any guideline.
Read the full CAHS disclaimer
|
Aim
To guide Emergency Department (ED) staff with the assessment and management of hand trauma, including hand lacerations, nail bed injuries and soft tissue injuries.
For the management of fractures refer to Fractures - Hand - ED Guideline.
Background1,2
- Hand trauma is a common presentation in children
- Injuries include lacerations, nail bed injuries, soft tissue injuries, dislocations and fractures
- At PCH, any injury which may affect normal hand function should be referred to the Plastic Surgery team
Key points1,2
- Hand injuries tend to have a bimodal distribution with toddlers typically presenting with lacerations and soft tissue injuries and adolescents with fractures.
- Crush injuries are common in younger children as they explore their environment with their hands. These can cause minor lacerations, nail bed injuries, subungual haematoma and fractures.
- Older children tend to have injuries from sport, sharp tools or equipment.
Assessment
- Thorough examination of normal hand function is important to detect underlying fracture, tendon, vessel or nerve injury.
Examination1,2,3
- Compare both hands and look for bruising, erythema, swelling and deformity
- Passive and active range of movement of all joints in hand and wrist should be examined. Testing against resistance may identify ligamentous injury
- Rotational deformities may be more obvious when the patient makes a fist
- Palpate for obvious areas of tenderness
- Assess for any neurovascular compromise
Investigations
- X-ray specific areas of focal bony tenderness or if risk of foreign body.
Management
Initial management
- Pain management - refer to Analgesia – ED Guideline
- Haemostasis
- If open fracture, bite or grossly contaminated wound, refer to Antibiotics – ED Guideline
- Review Tetanus Vaccination history, if not up to date refer to Tetanus Prone Wounds – ED Guideline
- Keep nil by mouth if referral to plastic surgeon is required
Further management1,2,3,4
- Simple soft tissue injuries are managed symptomatically
- See Fractures - Hand - ED Guideline if X-ray shows a fracture
|
Simple Skin Avulsion
- A simple skin avulsion of the nail or pulp, if smaller than the size of the nail will heal very well
- Apply a simple dressing (non-adherent) which can be trimmed at the edges as the wound heals.
|
|
Burst Lacerations of the Pulp
- If the laceration is less than half the circumference of the digit, apply Steristrips®
- If the laceration involves more than half the circumference, sutures will be necessary
- Majority of injuries do not require referral
|
|
Nail Bed Injuries
- Nail bed injuries should be referred to the plastic surgical team if:
- There is a suspected laceration of the nail bed
- Nail bed lacerations should be suspected where there are lacerations across the eponychial fold (where the proximal part of the nail disappears under the skin), or transverse lacerations of the nail which extend onto the skin on either side of the nail
- The nail is avulsed from the eponychial fold
- An underlying crush fracture is noted on X-ray
- These injuries require surgical intervention to prevent future nail deformity and infection
|
|
Subungual Haematoma
- The severe pain of a subungual haematoma may be relieved by trephination (creation of a small hole) at the base of the nail, but only after an underlying fracture has been ruled out by X-ray (if a fracture is present, seek advice from the plastic surgical team)
Trephination
- Prior to trephination, paint the nail with iodine solution, and then gently create a hole through the base of the nail through which the underlying haematoma can drain
- The hole can be bored by means of rapid twirling with a 23G needle or by the time-honoured method of heating the tip of a paperclip over a flame and then applying gentle pressure until the tip of the paperclip passes just through the nail
- Apply antiseptic ointment and a simple dressing
- Prophylactic antibiotics are not required
- Instruct the patient to keep the finger dry for three days
- A simple aluminium finger splint may provide some protection
|
|
Fingertip Fractures
- With crush injuries of the tip of the finger, soft tissue injury is more important than bony injury
- Generally, fractures of the tip of the distal phalanx require no treatment other than symptomatic buddy strapping or an aluminium finger splint
- However, if there is associated nail bed injury or pulp laceration, the fracture is a compound fracture and an opinion should be sought from the Plastic Surgery team
Antibiotics may be needed. Refer to Antibiotics – ED Guideline
|
- Lacerations caused by sharp objects (e.g., broken glass) are at increased risk of associated tendon injury
- Examine joint movement carefully
- Any suspicion of tendon laceration should be referred immediately to Plastic Surgery team
- Keep the patient nil by mouth while awaiting hand surgeon review
|
|
Stump Care
- Irrigate with saline to decontaminate
- Cover with sodium chloride 0.9%-moistened sterile gauze
- Control bleeding with direct pressure
- Splint and elevate hand
|
|
Care of the amputated part
- Irrigate with saline to decontaminate
- Wrap in saline-moistened sterile gauze
- Place in a watertight plastic bag
- Place bag in a container of ice water
- Consult with Plastic Surgical Team urgently
|
- Isolated dislocations are rare in children because their ligaments are stronger than bone, and trauma sufficient to induce dislocation in adults invariably results in bony fracture in children – refer to Fractures - Hand guideline.
- If a true dislocation is seen, it may be reduced in ED under nerve block +/- sedation. Refer to plastic surgery if irreducible.
- Immobilise appropriately post reduction (thumb spica or buddy strap) and follow up in plastic surgery hand clinic.
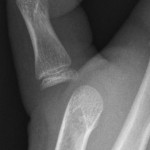
Thumb dislocation
|
References
- Sullivan, Matthew A et al. “Pediatric Hand Injuries.” Plastic surgical nursing : official journal of the American Society of Plastic and Reconstructive Surgical Nurses vol. 36,3 (2016): 114-20.
- Nellans KW, Chung KC. Pediatric hand fractures. Hand Clinics. 2013 Nov;29(4):569-578
- Yeh PC, Dodds SD. Pediatric Hand Fractures.Tech Orthop 2009; 24: 150-162
- Rang M, Pring ME, Wenger DR. Kluwer W, Rang's Children's Fractures Fourth edition. Wolters Kluwer, 2018
| Endorsed by: |
Clinical Practice Advisory Committee |
Date: |
Apr 2023 |
This document can be made available in alternative formats on request for a person with a disability.